Blog
Welcome to Brain Central.
Funding provided, in part, by the Government of Ontario.
- Home
- Blog

Supporting the Elder Brain Talk: Challenging Beliefs about Cognitive Aging, Dementia and Care
May 20, 2025
At our Supporting the Elder Brain public talk in March, the final event in our 2023–24 Brain Health Across the Lifespan series, a panel of experts came together to explore a question on many minds: How can we best support our brain health as we grow older? This thoughtful conversation wove together practical advice, personal […]

Philanthropy and the power to ignite research and innovation
December 19, 2024
“Some say we live in an era of polycrisis, a state of risk where multiple crises intersect to amplify their collective impact. In such a world, if we are committed to the well-being of Canadians and the country is to flourish, we need a broadly-shared effort. Building Canada’s future needs political, social and economic forces […]

Debunking Brain Health Myths: Insights from ‘Optimizing the Adult Brain’
December 11, 2024
The brain is one of the most intricate and vital organs in the human body, yet many misconceptions about brain health persist. During the recent “Optimizing the Adult Brain” public talk, experts in neuroscience, psychiatry, and community health addressed some of these myths, offering evidence-based perspectives to guide us toward lifelong brain wellness. Myth 1: […]

Take Care of Your Brain – Six Tips for Brain Health
September 23, 2024
Caring for your brain health and mental well-being is just as important as looking after your physical health. OBI’s brain tips offer simple solutions that can be implemented in daily life to nurture brain health and support yourself or your loved ones. Here are six tips on how to take care of your brain. Sleep: A […]

Nurturing the Developing Brain: A Holistic Approach Explored in Our Public Talk
September 09, 2024
On June 17, 2024, we launched the 2024-25 Brain Health Across the Lifespan series with the “Nurturing the Developing Brain” public talk. The event began with a smudging ceremony led by Elder Kerrie Moore, establishing a respectful and grounded atmosphere for the discussions that followed. Integrating Diverse Perspectives on Brain Health Our panel, comprising a diverse group […]

Insights from OBI’s ‘Eat and Play for Brain Health’ Public Talk
April 17, 2024
OBI’s 2023-24 Public Talks series, Brain Health Basics, concluded on a vibrant note with the engaging and insightful ‘Eat and Play for Brain Health’ talk held on Tuesday, March 26, 2024. This session delved into simple yet profound ways to support brain function in everyday life, emphasizing the crucial role of community, food, and social […]

OBI Public Talk: Sleep and Relax for Brain Health
February 16, 2024
“Really good sleep on a consistent basis affects your ability to optimize your performance at work, and it impacts your relationships with friends and family around you.” – Ontario Brain Institute Vice-Chair Heather Chalmers, in her introductory remarks to our recent Public Talk ‘Sleep and Relax for Brain Health’ In an era where burnout and […]

Generous investment reaffirms Ontario’s commitment to brain health
January 26, 2024
A message from Dr. Tom Mikkelsen, OBI President & Scientific Director As you no doubt have heard, the Government of Ontario recently announced a commitment of $65 million dollars to support the Ontario Brain Institute (OBI) in its work to accelerate solutions that improve brain health. It also paves the way for the establishment of […]

Move Your Mind: The Link Between Movement and Brain Health
December 18, 2023
“I got a video from a mom showing me her child is actually playing tennis. And the testimonial from the child is like, ‘Now I feel normal.’ And that’s the best feeling that we can ever have.” Sarah Lambert, neurotechnology entrepreneur New links between body and mind are being uncovered all the time. We discussed […]
Precision Medicine: Improving Tomorrow’s Health Today
October 31, 2023
““Each child has a story, and we have to listen to that story, and we have to help that child (and that family) construct that story so it starts to make sense” Dr. Peter Szatmari What if, instead of providing a blanket treatment for those impacted by brain conditions, healthcare providers were able to go […]

Thriving Beyond Labels and Overcoming Stigma: Perspectives on Living with OCD & ADHD
March 09, 2023
N1, diagnosed with ADHD as an adult, completed a PhD in neuroscience. They have worked closely with research programs carried out in partnership with the Ontario Brain Institute. N2 is currently an undergraduate student at York University. They have been living with OCD since childhood – and have brought their lived experience to the Youth […]

How to Have a Social Life as a Teen with Epilepsy
March 09, 2023
My name is Kieran, and I am a grade 11 student. I have epilepsy. I have approximately 5 seizures per day. I experience seizures every day at school and have since I started school a decade ago. I also have a visual disability and autism. In order to attend high school, I have had to […]

Returning to work after a stroke: Workplace stigma & the value of empathy for others
March 09, 2023
“Having a stroke happens in the snap of a finger. You go from being hard-working and being in reasonably good shape to having to make many life-changing decisions.” My name is Ron, and I am a stroke survivor. Since my stroke, I have been involved with March of Dimes, Patient Visitation (previously known as Peers […]

“We need to listen to women and believe what they are saying”
March 07, 2023
OBI Public Talk on Women’s Brain Health “These women are so wise, empathetic, and passionate about their work, and I feel truly ‘seen’ for the first time in a long time,” said one attendee after an OBI public talk on December 7, 2022. Panelist Profiles From normalizing discussion of brain disorders that affect women such […]

Meditation – A simple way you can destress and calm your mind
October 06, 2022
“The quieter you become, the more you are able to hear” – Rumi When you hear the word ‘meditation’, what ideas or thoughts first come to mind? Is it that it’s difficult? That it takes too long? Maybe that it’s even inaccessible and for the ultra-disciplined? Well, meditation can be uncomplicated, quick, accessible, and can […]

The Research Journey and the Crucial Role of Patient Engagement
July 12, 2022
Our patient and community members’ desire to gain an understanding of the scientific research journey inspired our most recent Discovery Starts With You Series event. In May 2022, the Ontario Brain Institute held a talk, co-hosted with Dr. Samantha Yammine or “Science Sam” about the research journey. She unraveled the importance of patient involvement in […]

Announcing OBI’s Open Call for Integrated Discovery Programs
June 01, 2022
After marking a decade of excellence in brain health, the Ontario Brain Institute is looking to the future. We’re mapping out the next phase of our 30-year vision to improve the lives of the one in three Ontarians impacted by a brain disorder. A major piece of our go-forward plan is an open call for […]

Communication challenges with aphasia can exacerbate caregiving stress
May 05, 2022
Until last week, few people knew the term aphasia. The recent announcement that the actor, Bruce Willis, has stepped back from his acting career, due to aphasia, has raised a much-needed spotlight on persons living with aphasia and their families. According to aphasia.ca, Conservative estimates suggest that more than 100,000 Canadians are living with this […]
How to Transform a Promising Idea from the Lab to Life
June 09, 2021
OBI is working towards creating an inclusive society for neurodiverse people that accommodates a vast range of needs. In the last decade alone, we have seen plenty of promising tech coming out of Ontario’s neurotech cluster. Entrepreneurs and researchers are coming up with creative solutions to directly address barriers that exist for people with brain […]
Why Patient Engagement Matters in Improving Brain Health?
May 05, 2021
1. Lived experience offers valuable insight on what matters “Being a part of OBI’s Patient Advisory Committee has provided me the opportunity to increase my own knowledge base while being able to share my opinions and thoughts – the ability to contribute a broader personal perspective, based on my lived experience and professional experience […]
The Potential of Data Sharing: What Data Means for your Brain Health
February 25, 2021
“As the world has grappled with a global pandemic, we have faced much uncertainty and many challenges in our society and our economy. In dealing with these issues, however, we have also been presented with an opportunity – the chance to rethink outdated conventions and renew the way we do business as we rebuild our […]
The Potential of Data Sharing: What Data Means for your Brain Health
February 18, 2021
“As the world has grappled with a global pandemic, we have faced much uncertainty and many challenges in our society and our economy. In dealing with these issues, however, we have also been presented with an opportunity – the chance to rethink outdated conventions and renew the way we do business as we rebuild our […]
Trexo Robotics – Benefits during COVID – Meet Jacob
September 11, 2020
Jacob’s case study is quite an important one to share. Jacob has a milder form of Cerebral Palsy, where he can walk by himself in a walker, but needed help in improving his gait. He also has some speech difficulties, but his cognition is perfectly fine. Jacob’s family got the Trexo in November 2019 hoping […]
Three Takeaways – Pain in Children: What we don’t know can hurt them
July 17, 2020
“We don’t have to let kids suffer in silence” said Ontario Brain Institute’s President & Scientific Director, Tom Mikkelsen, as he opened one of OBI’s Public Talks, “Pain in Children: What we don’t know can hurt them”. The event featured four speakers, each with a unique expertise when it comes to pain experienced by children, […]
OBI-GEEK – Brief Intensive Case Management – Acquired Brain Injury Ontario Brain Injury Association (Nipissing District)
July 17, 2020
Severe brain injuries can dramatically alter the trajectory of someone’s life. Take the case of Michael, not his real name, who suffered from a severe brain injury as the result of a motor vehicle collision. His injury meant that he struggled with poor memory, impulsivity, dysarthria, chronic pain, emotional dysregulation, poor money management and many […]
OBI-GEEK – Educational Pathway to Employment Christian Horizons (Toronto)
July 17, 2020
In 2019, the Educational Pathway to Employment Program, a partnership between Christian Horizons and Humber College, was awarded one of the Ontario Brain Institute’s (OBI) Growing Expertise in Evaluation and Knowledge Transition (GEEK) initiative grants. The Educational Pathway to Employment program is a post-secondary nine-month culinary certificate program for people with disabilities. The hands-on specific training […]
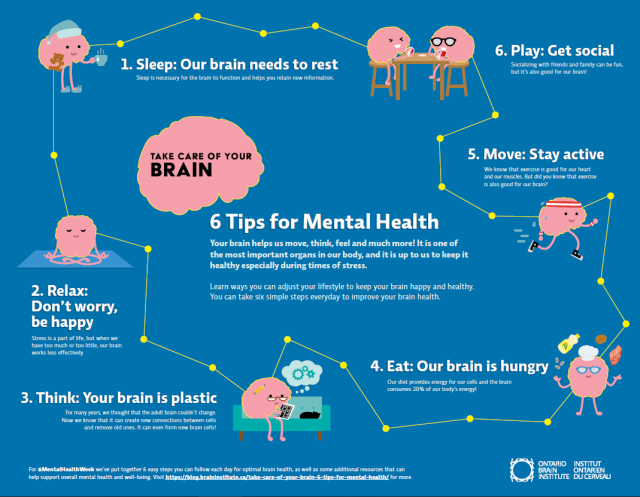
Take Care of Your Brain – Six Tips for Brain Health
May 04, 2020
Caring for your brain health and mental well-being is just as important as looking after your physical health. OBI’s brain tips offer simple solutions that can be implemented in daily life to nurture brain health and support yourself or your loved ones. Here are six tips on how to take care of your brain.
Team Science: the key to unlocking scientific advancement
August 27, 2019
You know the phrase, “two heads are better than one”? Sometimes, many heads are needed to solve a problem; this is especially true for the problems we face in brain health. For this reason, OBI believes in a collaborative model to solve complex problems by forming sustainable partnerships in research, commercialisation and care. In this […]
Adapting To New Normals Through Neurotechnology
June 07, 2019
We take brain health for granted. We tend not to think about it until something changes and a once simple task becomes difficult. Remember when you incurred a sports injury and were on bed rest for a few weeks; the time when you were feeling low and struggled to reach out to one of […]
After the top 10: bringing the community priorities to life
February 11, 2019
It’s been over a year since the final workshop of our neurodevelopmental disorder Priority Setting Partnership (PSP). This seminal moment marks the day when patients, family members, and front-line care providers came together and reached consensus on a top 10 list of research priorities for the research community. While all PSP initiatives culminate in a […]
Towards a learning healthcare system through collaboration
September 07, 2018
There is no question that the looming grey tsunami of the ageing population in Ontario has significant implications with regards to healthcare services. A key concept which is emerging is the opportunity to foster and maintain brain health across the lifespan where optimal performance and quality is sustained. While much focus has been on the […]
Sharing Caregiving Strategies to Address Risky Behaviour Changes in Dementia
March 29, 2018
Caring for someone with dementia is a long and challenging journey. Over the course of this disorder memory, cognitive function and other abilities deteriorate. Behaviour can also change over time in ways that are completely out of character for that person. For instance, the person with dementia may display aggressive behavior or get angry and […]
A Holistic Way to Think About Our Health and Reframe Disability
March 05, 2018
No one likes to be defined by an illness, disorder or disability – even when we are a patient. Our ‘health’ is not only based on our biology, but also by our relationships with friends and family and our ability to do the things we enjoy. Researchers Drs. Peter Rosenbaum and Jan-Willem Gorter from our […]
Message from the President and Scientific Director
December 15, 2017
Dr. Tom Mikkelsen, President and Scientific Director of the Ontario Brain Institute (OBI), reviews the accomplishments and innovations of OBI over the past 5 years, and how this lays the foundation for even greater impacts in brain research, commercialization and care in our next phase.

Brain-CODE – An Engine for Collaboration
December 15, 2017
The Ontario Brain Institute (OBI) builds collaborations between Ontario neuroscientists so that they can combine their diverse expertise and resources to better understand brain disorders and translate these discoveries into new tools and treatments.

Grooming Entrepreneurial Talent for Great Health Returns
December 15, 2017
Ontario has one of the highest concentrations of neuroscientists in the world, creating an opportunity for a thriving industry around the development of neurotechnologies to treat brain disorders. However, a study of Ontario’s ability to develop a neurotechnology cluster highlighted two obstacles; a lack of access to capital and insufficient managerial talent.

Building Networks Fundamental to Improving Health Impacts
December 15, 2017
Since the inception of Ontario Brain Institute (OBI) in 2010, we have been forging ahead with a singular mission – improve the lives of the over one million Ontarians living with a brain disorder. OBI’s work focuses on three key areas: engaging patients in research; catalyzing evidence into practice and promoting a culture of evaluation. […]

Enhancing the Neuroscience Research System through Strategic Collaborations
December 14, 2017
Brain disorders affect one in three Ontarians and the direct cost to the province exceeds $4 billion each year. The indirect costs from work missed and the emotional costs for families are incalculable and create an urgency to address brain health by means of innovation and translational research that can improve the quality of life […]

Setting the Stage for Deep-Data Analysis and Innovation
December 04, 2017
“With great power comes great responsibility” – Ben Parker. Ontario Brain Institute’s (OBI) researchers collect ‘deep data’ using scientific and clinical tools like behavioural tests, neuroimaging and genetics. By bringing these data together in Brain-CODE, we can develop a holistic approach to understanding brain disorders. A recent report, “Dementia Research and Care: Can Big Data […]

Inventiveness Accelerates Drug Discovery Process- A smart shortcut to developing new drug treatments for Parkinson’s disease
November 16, 2017
It takes almost a decade and billions of dollars to develop a drug for brain disorders. Furthermore, 88% of those drugs fail clinical trials because of their lack of efficacy and safety1. The entire process is not only daunting but very costly, in terms of time and money. But, what if there was a way […]

Your Questions Answered: Neurodevelopmental Disorder Priority Setting Partnership
October 18, 2017
We asked people living with neurodevelopmental disorders, their families, friends, carers, and healthcare professionals to list questions they had about diagnosis, therapies, care, and other interventions for neurodevelopmental disorders. After receiving about 1300 questions from 300 individuals across Ontario, we grouped them by topic, and checked against published research to see if they have already […]

The Ontario Brain Institute assembles province’s Brain Power at Queen’s Park
September 22, 2017
By Shaalee Sone, Outreach Intern, Ontario Brain Institute The Ontario Brain Institute (OBI) held “Meet Ontario’s Brain Power” on September 11 at Queen’s Park. The day served to showcase OBI’s work that has positioned Ontario as a world leader in brain research, commercialization and care.

Physical activity protects us from losing brain function
September 21, 2017
By Shaalee Sone, Outreach Intern, Ontario Brain Institute As our population ages, Canadians are looking for ways to prevent dementia. As of 2010, there are 136 000 Ontarians living with a confirmed diagnosis of dementia. In addition to the impact on individuals and their families, the direct cost to the Ontario health care system is […]

Reducing the stigma of overdose and increasing awareness
August 31, 2017
By: Shaalee Sone, Outreach Intern, Ontario Brain Institute There is a tendency to categorize people who have died or been injured by overdose as “others,” but overdose can affect anyone – our friends, our parents, our siblings, our children and even ourselves. The impact of overdose extends beyond each individual, onto their family, their friends […]

Another side of cerebral palsy: the genetic story
August 15, 2017
Photo credit: Veronica Rousseau By: Shaalee Sone, Outreach Intern, Ontario Brain Institute In the age of genomics we are racing to uncover what our genes say about us. If we had the ability to read our genetic code and learn what’s in store, we could play to our strengths and prepare for our limitations. One […]
OBI’s Founding President and Scientific Director Named Officer of the Order of Canada
January 12, 2017
A message from Dr. Tom Mikkelsen, President and Scientific Director The Order of Canada is one of Canada’s highest civilian honours. It recognizes an individual’s outstanding achievement, dedication to the community, and service to the nation. 2017 marks Canada’s 150th anniversary and the 50th anniversary of this unique award. During this especially notable year, we […]
Message From The President And Scientific Director
November 29, 2016
Research in the 21st century is remarkably different than it has been in any previous era. This is especially true in the world of brain research.

OBI’s Public Talks: Moving Beyond Academic Forums And Science Communication
November 29, 2016
By: Lucia Kwan, Research Programs Intern, Ontario Brain Institute Do you know someone living with autism, dementia, or depression? Chances are you do. In fact, we know that one in three Canadians have or will develop a brain disorder in their lifetime. In Ontario alone, there are at least 135,000 individuals living with dementia as […]

Connecting Ontario’s Strengths For Concussion Research and Care
November 29, 2016
By: Johnathan Tran, Informatics & Analytics Intern, Ontario Brain Institute It’s easy to take for granted how important a healthy brain is until it isn’t. Made up of billions of interconnected cells, the human brain, encased in a solid boney skull, is remarkably resilient but this does not make it immune to injury. When […]
Message From Dr. Tom Mikkelsen, President And Scientific Director Of OBI
June 09, 2016
At the risk of stating the obvious, the brain is complex and brain disorders represent a large and growing concern for global health. It’s likely that we all agree on the scale and importance of this problem, but like all big problems, there are many different approaches to reach a solution.

Patients’ Priorities: It’s A Very Good Place To Start
June 09, 2016
By Meredith Bibbings, OBI Intern, Research The most effective initiatives are responsive to the needs of those who stand to benefit from them. In research, this can mean understanding the patient, policy, commercialization, and care provider landscape.
Taking Control Of Epilepsy With Diet Therapy In A Pill
June 09, 2016
By: Aparna Shukla, OBI Intern, Informatics & Analytics Imagine having to live with sudden changes in sensory perception, loss of consciousness and involuntary muscle convulsions. More than 50 million people worldwide and approximately 90,000 people in Ontario live with epilepsy, including nine-year-old Adam.
Message From Dr. Tom Mikkelsen, President And Scientific Director Of OBI
December 02, 2015
Your brain is always changing. It is constantly processing information from your body and making sense of the world around you. And in doing so, your brain itself is changing. In fact it continues changing throughout your lifetime. You experience this change with every new skill you learn, and every old memory you forget. Neurogenesis, […]

Helping Companies Get Over Their First Hurdles
November 23, 2015
Dr. Ron Gonzalez is passionate about taking science out of the labs and putting it into practice. As a result of his success in doing just that, today he’s the President of Avertus Epilepsy Technologies Inc. (Avertus): a company focused on improving the lives of people with epilepsy through the development of a wearable headset […]

International Data Linkages For New Possibilities In Autism Research
November 23, 2015
OBI catalyzes the impact of brain research in Ontario by increasing collaboration among researchers, doctors, patients and their advocates, and industry partners. A key ingredient to collaboration is, of course, sharing. At OBI, a cornerstone of effective research collaboration involves sharing large quantities of data. In order for this to be done effectively, it must […]

Expanding The Borders Of Research Through Cross-Disorder Collaborations
November 23, 2015
While autism, epilepsy, or depression may at first seem worlds apart, there is benefit in studying these and other brain disorders together. Each condition has unique traits, but there is often overlap. For instance, people living with autism may experience depression and people living with cerebral palsy may have seizures. Brain research is inherently complex – different […]

Brain Injury: Planting the Seeds for Greater Awareness
June 22, 2015
Facing the realities of a new life after experiencing a brain injury can be a source of struggle, pain, and a journey of self-discovery. Simple pleasures like playing with your children, making a delicious meal, or biking with a friend can be stripped away in an instant with injuries to the brain following motor vehicle […]
Message from Dr. Donald Stuss, President and Scientific Director of OBI
May 12, 2015
Of all the mysteries in neuroscience, memory is among the most heavily researched. There is an important distinction between semantic( basic general knowledge; e.g., Paris is the capital of France) and episodic, or personal, memories (tied to time, place, people; e.g., last Saturday night, my wife and I had a fantastic dinner of mushroom risotto […]

Filling Gaps in Ontario’s Neurotechnology Sector with Phantoms
May 04, 2015
Imagine you are treating someone with a suspected traumatic brain injury—what if you could have a non-invasive look inside their brain to assess the damage and decide on treatment? Ontario-based Tessonics Inc. developed a device that could do just that, but the next challenge was how to properly calibrate the device to ensure reliable and […]

Alzheimer’s Awareness Month: Influential Discoveries of 2014
January 19, 2015
By Bryan Jenkins, OBI Intern, Research Programs At the end of 2014, many of us – with the help of certain social media websites – were reflecting upon the past year of our lives. It was a big year for neuroscience and brain health, following from our proclaimed ‘Year of the Brain’. In this post […]
Give Your Brain A Holiday
December 10, 2014
Message from Dr. Donald Stuss, President and Scientific Director of OBI
October 10, 2014
Understanding who you are, deciding how you behave, experiencing love and laughter — the brain is key to these behaviours. Perhaps the most important brain region underlying these functions is the frontal lobes, the area of the brain most closely tied to these highest functions.

Addressing Dementia Research And Care: Can ‘Big Data’ Help?
October 09, 2014
We live in a world of big data which can serve as a particularly useful tool for health systems to gain a better understanding of patients and their needs across large populations. With appropriate use, big data has the potential to advance health research and help healthcare providers personalize care; however, this has been largely […]
Looking at New Ways to Improve the Patient Experience
July 02, 2014
By: Tiffany Scarcelli, MSc, OBI Management Fellow When a child becomes seriously ill, there are many concerns, thoughts, and fears that arise in both the child and their family upon their first hospital visit. Will my child respond to treatment? Will they get the best care possible? What many people do not realize is that […]

Bringing Together the Brightest Minds to Beat Depression
April 24, 2014
By: Dipa Basu, PhD, OBI Management Fellow 1 in 10 Canadians will be affected by depression at some point in their lives. The remaining 9 will know someone who is affected. Depression is a mood disorder which can become isolating and debilitating, and in some cases, even life-threatening. However, innovative research within this field is […]
Message from Dr. Donald Stuss, President and Scientific Director of OBI
March 25, 2014
86 billion: that is the number of neurons, or cells, estimated to make up the human brain. Within each cell there is a universe of complexity and activity. But the remarkable abilities of the brain to think, remember, respond, and feel, cannot be explained by just scaling up the individual actions of each cell. It […]
Your Brain Health: Practicing What You Preach
March 25, 2014
By promoting brain awareness across Ontario, OBI is helping people take charge of their own brain health. Need some inspiration? OBI staffers reveal their own brain-health tips.

The OBI Celebrates Interns and Entrepreneurs
January 03, 2014
By: Christopher Smith, PhD,OBI Intern with the Industry Relations team As a recent PhD graduate people always ask me ‘what’s next?’ I believe this is possibly the most common question asked to new graduates, but it is also the most difficult to answer.

Your Brain on Holidays
December 17, 2013

“A Brain is a Beautiful Thing to Share”
October 09, 2013
For many, learning about science is like hearing Klingon: you may have a (very) vague idea about what’s going on, but you’d be hard-pressed to explain it. That’s why at Queen’s University, steps are being taken to bridge this gap and reach out to the public.

A personal touch to understanding neurodevelopmental disorders
September 18, 2013
Researchers are focusing on the individual to gain deeper insight into the common, underlying causes of neurodevelopmental disorders.

A guiding hand to steady tremors
September 18, 2013
A team of experts has combined a new technology with an old treatment to create a better way to still tremors and restore limb function.

Message from Dr. Donald Stuss, President and Scientific Director of OBI
March 11, 2013
It’s Brain Awareness Week 2013 – a time to think about the promise of brain research and how it’s helping all of us take practical steps towards healthier brains and a healthier future.
Brain-CODE embraces Privacy by Design (PbD) for a Win-Win Solution!
October 29, 2012
By: Ann Cavoukian, Ph.D. Privacy by Design (PbD) Privacy by Design (PbD) is a framework I developed in the ’90s to shift the conventional method of privacy protection from a reactive regulation and compliance model to a proactive preventative model. Fast forward to today – advances in technology have become faster and more robust; our […]

Message from Dr. Donald Stuss, President and Scientific Director of OBI
September 10, 2012
The brain. It drives our intelligence, our feelings, our ability to interact, to walk and talk, remember the good times, plan for the future, and care for ourselves and each other. It is the core of our lives and our world.
CIHR’s New Funding Initiative
August 09, 2012